CureScience works alongside organizations like these to ensure patients have access not only to advanced scientific insights but also to the human support systems that make a difference every day.
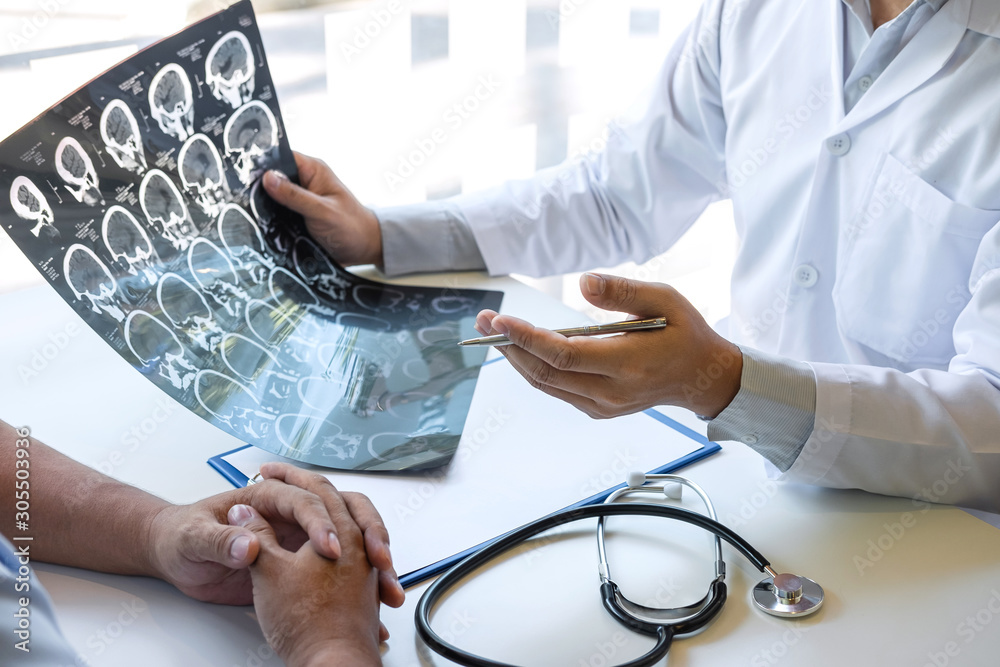

Ancora is an AI-powered platform designed to help patients and clinicians better understand complex cancer data. By organizing clinical, genomic, and treatment information into a more actionable format, Ancora supports more informed decision-making and personalized care pathways.
A nonprofit focused on applying precision medicine in real time by connecting patients, physicians, and researchers. Cancer Commons helps interpret molecular data and identify personalized treatment options, including clinical trials and emerging therapies.

Provides access to comprehensive cancer care, including integrative and advanced treatment approaches, for patients seeking additional options beyond standard pathways.
Immunocine offers a personalized immunotherapy that utilizes a proprietary Double Loaded dendritic cell technology to help your immune system detect and fight cancer. Our approach combines scientific rigor with personalized immunotherapy to address cancer as an immunological disorder.

Advanced Diagnostics & Next Generation Cellular Treatments

Coming Soon.

Coming Soon.
When you support CureScience, you help advance research, strengthen patient engagement, and bring hope closer to real outcomes for patients and families.